 
To avoid touching the lens, one should switch hands or have an experienced assistant perform scleral depression to reach the peripheral vitreous on the opposite side. In phakic patients, one should be mindful of the crystalline lens while trimming the vitreous cone, especially when reaching across the lens with the cutter (Figure 1). Rarely, one might need to use a pick or scissors to do the same if one fails with the cutter. 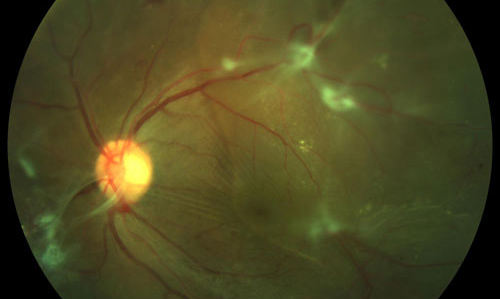
If this seems difficult, one can slide the cutter tip through the adjacent trimmed edge of the cone to lift the adherent vitreous. In such cases, one should apply a little more suction with the cutter to release the vitreous from the surface of the retina. In some patients, the peripheral vitreous may be tightly adherent to the retina in some areas. In phakic patients, surgeons should avoid reaching across the lens with instruments, especially beyond the equator. The cutter port should face the surface of the vitreous while the cone is trimmed.įigure 1. Removal of vitreous should begin around the two superiorly placed sclerostomies and then proceed to the vitreous cone, which should be trimmed in the midperiphery, or wherever there is maximal separation between the vitreous and the underlying retina, using the highest cut rate and least amount of suction possible. One should avoid going directly to the nerve to induce a PVD or initiating membrane dissection until the peripheral vitreous cone has been trimmed, as pulling on the vitreous at the nerve without trimming the peripheral vitreous cone can lead to iatrogenic tears in the peripheral retina. The first step in any case of TRD should be to trim and release for 360° the peripheral vitreous cone. In TRDs, the vitreous is usually detached in the midperiphery, but multiple attachments remain at the posterior pole, thus forming a vitreous cone. Most cases of RRD will have a complete PVD, whereas this is uncommon in TRDs. The vitreous in diabetic and other TRDs differs significantly from the vitreous in an eye with routine rhegmatogenous retinal detachment (RRD). Attention is then turned toward tackling the peripheral vitreous (Video /?v=opool.) If vitreous hemorrhage is present, it is cleared in the standard fashion. Color and red-free photographs are also helpful and should be reviewed the night before surgery. Spectral-domain optical coherence tomography (OCT) imaging is helpful in assessing the level and severity of the membranes and can provide clues regarding the location of potential spaces where safe dissection or initiation of membrane removal can be performed. All strategies employed are geared toward avoiding breaks in the ischemic, fragile retina. Therefore, the chief surgical goal of TRD repair includes complete release of the hyaloid with dissection of all tractional fibrous membranes. This cascade of events explains why an eye in a patient with diabetes is protected from a TRD if a complete posterior vitreous detachment (PVD) has occurred before any evidence of neovascularization. With time, the vitreous can contract and exert tractional forces on the retina via these fibroglial connections, leading to a TRD. Subsequently, glial cell proliferation encases these vessels in fibrous tissue. The new vessels then break through the internal limiting membrane and grow along the surface of the retina and into the scaffold of the posterior hyaloid face. These growth factors lead to the development of fragile new vessels from the existing retinal veins. Progressive retinal ischemia leads to pathologic secretion of growth factors, especially VEGF. Tractional retinal detachment (TRD) may occur in a number of conditions, such as proliferative diabetic retinopathy (PDR), retinal vein occlusion, trauma, sickling hemoglobinopathies, and retinopathy of prematurity. 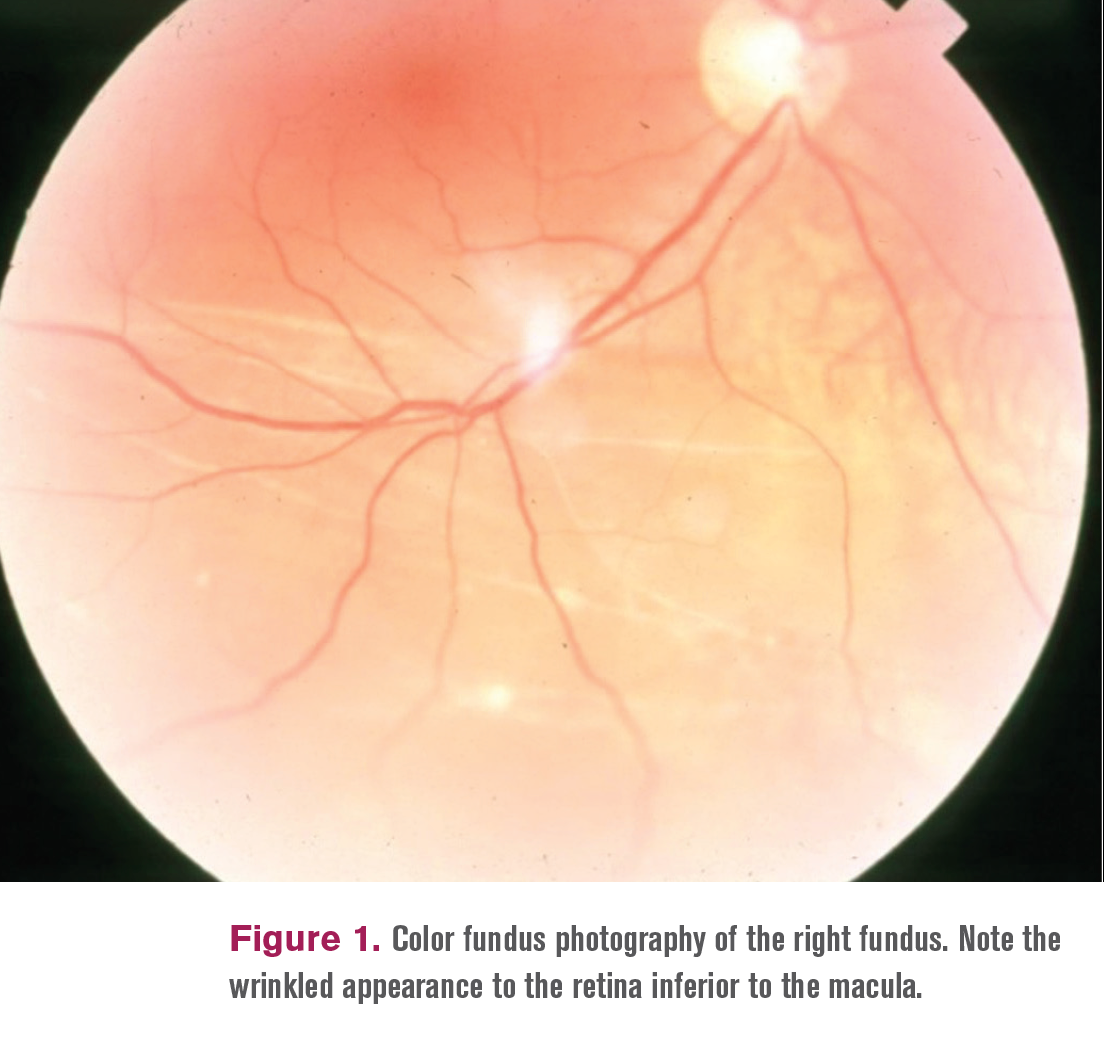
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
